Serviços Personalizados
artigo
Indicadores
Compartilhar
SMAD. Revista eletrônica saúde mental álcool e drogas
versão On-line ISSN 1806-6976
SMAD, Rev. Eletrônica Saúde Mental Álcool Drog. (Ed. port.) vol.15 no.2 Ribeirão Preto abr./jun. 2019
http://dx.doi.org/10.11606/issn.1806-6976.smad.2019.000431
ORIGINAL ARTICLE
DOI: 10.11606/issn.1806-6976.smad.2019.000431
Sharing care in psychosocial care: perception of workers and users
Intercambio de cuidados en atención psicosocial: percepción de trabajadores y usuarios
Rafael Pasche da SilveiraI; Daiana Foggiato de SiqueiraI; Amanda de Lemos MelloI; Fernanda de Almeida CunhaI; Marlene Gomes TerraI
IUniversidade Federal de Santa Maria, Santa Maria, RS, Brasil
ABSTRACT
OBJECTIVE: understand the
perception of workers and users about the sharing of care to the user egress
from a Psychosocial Inpatient Unit with referral to a Psychosocial Care Center.
METHOD: qualitative research, developed in a
Psychosocial Internment Unit and a Psychosocial Care Center. The interviewees
were 15 professionals and 10 users.
RESULTS: the
referral and the access of the users to the substitutive services and the
guidelines referring to the patient’s hospital discharge as challenges for the
sharing of the care were evidenced. In addition, the reception, the high
attendance and the link with substitutive services, presented possibilities for
the sharing of the care.
CONCLUSION: the importance of
care based on the principles of interdisciplinarity, intersectoriality and
integrality is observed.
Descriptors: Mental Health; Health Services Accessibility; Integrality in Health; Intersectoral Action.
RESUMEN
OBJETIVO: comprender
la percepción de trabajadores y usuarios acerca del compartir el cuidado al
egresado de una Unidad de Internación Psicosocial con encaminamiento a un
Centro de Atención Psicosocial.
MÉTODO: la
investigación cualitativa realizada en una Unidad de Hospitalización
psicosocial y un Centro de Atención Psicosocial. Los encuestados fueron 15
profesionales y 10 usuarios.
RESULTADOS: se presentaron
enrutamiento y fácil acceso a los servicios alternativos y directrices
relacionadas con el usuario del hospital alto como retos para el intercambio de
cuidado. Además, el anfitrión, asistido alto y el enlace con los servicios
alternativos, se presenta posibilidades para el intercambio de cuidado.
CONCLUSIÓN: señala la importancia de un cuidado guiadas los
principios de la interdisciplinario, intersectorial e integridad.
Descriptores: Salud Mental; Accesibilidad a los Servicios de Salud; Integralidad en Salud; Acción Intersectorial.
Introduction
The proposal of the Psychiatric Reform seeks strategies to reduce psychiatric hospitalizations and its actions are geared at providing care to the users. Among the proposals, there is the Psychosocial Care Center (PSCC), which is a primary and open-door service, an environment composed of workers from different nuclei offering care of diverse areas such as nursing, occupational therapy, physiotherapy, psychology, as well as medical consultations and social service. Besides specific services, there are different workshops and groups created in response to the user demands. This is the main mental health service of territorial base, becoming, therefore, fundamental in the share of care grounded on intersectoriality(1).
Assistance to users, according to the National Humanization Policy (NHP), can come from the organization in mental health networks, through shared care. It consists in the production of new modes of care and new ways of organizing the collective work so as to improve health work. Thus, sharing of responsibilities in health care aims at greater effectiveness through the autonomy of the individuals involved, strengthening shared responsibilities in management and care processes(2).
The NHP has sought to consolidate Mental Health Care Networks based on the principles of intersectoriality, comprehensiveness and interdisciplinarity. Intersectoriality is the articulation between health services and society. Comprehensiveness refers to the guarantee of the right of access to all spheres of health care, from assistance actions to activities of disease prevention and health promotion. Finally, interdisciplinarity appears as an overcoming of dichotomous thoughts in health care, contributing to the strengthening of the interaction between specialties(2-4).
Shared care based on these principles can be understood as a strategy for reducing the fragmentation of care based on the existing connections within a health network. It also enables teams to join different skills and make the care transcend beyond disease. Workers and managers, therefore, play a fundamental role in the construction of a mental health service that allows the development of shared care(5).
Knowing the context of change in mental health care through the history and the services that are active in the care network, the following question is raised: how does the sharing of care to the users leaving a psychiatric inpatient unit with referral to a PSCC take place? The relevance of this study is justified by the experience of multiprofessional residents enrolled in a Psychosocial Inpatient Unit (PIU) of a Teaching Hospital.
In this unit, re-hospitalization of users within short periods of time was observed, corroborating with studies that point to the phenomenon called "revolving door". This phenomenon consists in the frequent admission and re-admission of users in psychosocial hospitalization units, being a reason for concern that reflects flaws in the sharing of care(6-7). In view of this, the objective of this study is to understand the perception about the sharing of care of workers and users leaving a Psychosocial Hospitalization Unit with referral to a Psychosocial Care Center.
Method
This is a qualitative research, which appreciates the experience of relationships and the meanings that individuals attribute to certain phenomena(8). Two mental health network services of a municipality in the countryside of the state of Rio Grande do Sul, Brazil, that assist people with mental disorders, were the scenario of the study. One was the PIU of a large Teaching Hospital and the other as a PSCC II. The latter is one of the four PSCCs existing in the municipality, being the only one that receives cases of adult patients with psychiatric disorders.
The participants of the research were patients who had been discharged from the PIU and referred to the PSCC II and health workers from both services. Users referred to the PSCC from January 2015 to January 2016 were invited to participate in the study, based on the consultation of the PIU discharge records. Thus, the inclusion criteria were: men and/or women discharged from the PIU of the abovementioned hospital who were referred to the PSCC, with regular or irregular treatment in the service. The exclusion criterion was: users who were under the effect of some medication at the time of the interview or who had difficulty to communicate. The invitation was made from a previous contact via telephone call or face-to-face meeting in the PSCC.
Among health workers, those who worked at the PIU and who participated in the discharge of users and the PSCC workers who received the users referred from the PIU were invited to participate in the study. The inclusion criteria were: middle and higher level health workers who worked permanently in these services (Physicians, Nurses, Social Workers, Occupational Therapists, Psychologists, and Nursing Technicians) and residents of the Medical and Multiprofessional Residency Programs in Health (Nursing, Occupational Therapy, Social Work).As exclusion criterion: workers on leave of any kind or on vacations in the period of data collection. Thus, the corpus of the study was composed of eight university hospital workers, seven PSCC workers, and ten users who had undergone psychiatric hospitalization and were referred to the PSCC.
Data were produced from June to August 2016 through semi-structured interviews and were recorded with a digital recorder and later transcribed by the main investigator. The interviews lasted from twenty to thirty-five minutes and were held in the consultation rooms of the mentioned services. The triggering question used in the interviews of the PIU workers was: "how do you carry out the referral of users from the psychiatric unit to the PSCC?"; and to the PSCC workers was: "how does the embracement in the PSCC of users who were discharged from the psychiatric inpatient unit take place?"; and, to the users: "how was it for you to be discharged from the hospital and referred to the PSCC?". The collection ended when there was data saturation, that is, when information began to be repeated(9).
Thematic Analysis was used to analyze the data analyses, following the Operative Proposal(8), which is characterized by two levels of interpretation. The first interpretative moment consists in the historical context of the social group in question. The second interpretative moment represents the convergence with the empirical facts; it is the moment in which meanings and interpretations are found in the reports of the informants. In order to operationalize this second moment, the following steps were followed: organization of the data; horizontal and exhaustive reading of texts; final analysis and report, , completing the presentation of the results of the research.
Ethical aspects involving human beings were respected in accordance with Resolution Nº 466/2012 of the National Health Council(10). In order to maintain the confidentiality of the interviewees, the workers and users were identified by the letters W (workers) and U (users) followed by the number corresponding to the order of the interviews. The research was approved by the Research Ethics Committee under Opinion Nº 1,538,373/2016.
Results
Two interrelated categories were constructed from the analysis of the statements, namely: Challenges for sharing of care and Possibilities for sharing of care, according to Figure 1.
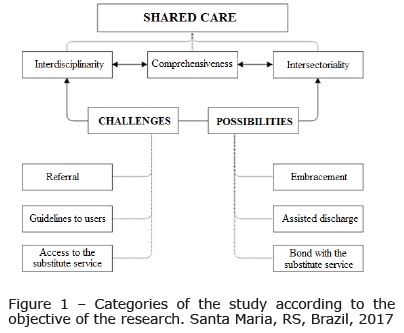
Challenges for sharing of care
Regarding the discharge of users and their referral to services in the mental health network, it was observed that not all workers participate in this process. Thus, those who carry out the referral do this through letters containing general explanations about the users. Actually, we don’t do this referral. We do not get this contact with the network. (W5); I was in the hospital there and the doctor called me and I was discharged. (U2); It is a document; it is not exactly a reference, nor counter-reference. But it’s a letter, a document, explaining the pathology, the medications in use, and requesting medical follow-up there [...] Patients sometimes lose their letters. (W7); I came here and told him that I was hospitalized; I showed them the document of discharge. (U3).
Some workers believe that referral through a document is not enough and they seek to make the contact via telephone. However, the users indicate that they do not receive guidance regarding the substitute service at the moment of discharge. I think it is important to continue following the case, through telephone contact [...] and sometimes, when I think it is necessary, important ... we send a written document; but it is usually done by telephone calls. (W4); We have a theoretical critique about the bureaucratization of the referral system, where you just give a paper to the patient and tell him to go to such a place at such address. This makes the contact more formalized, not so efficient according to the critique that we see. We try to solve this through a more personal, more professional contact of reference. (W6); No! I did not receive anything; I just thought it might be good for me to come to a service like this. (U7); I do not remember any guidance. They guided me here in the PSCC. (U10).
Workers report on how services should develop mental health care. In their opinion, the success of treatment is directly linked to the network that supports it. They recognize the weaknesses to which the services are exposed regarding access to the substitute service. This is a matter of intersectoriality, which is what we want, that services communicate with each other, knowing what the other has already done, knowing who is following up that case [...]. I am usually able to communicate with the PSCC, but I think the PSCC has no capacity to accomplish everything that would be needed, because there would be many users. The network is also sometimes unable to take care of all; it is a question of precarious social assistance in the municipality. (W4); There are all these other obstacles to ensure the referral and these other things, difficulty of access, socioeconomic issues, non-acceptance of treatment [...] many of our patients are not able to access the service because they are very poor, because of the places where they live, because of the precarious nature of transportation; in other words, various situations of social difficulty to access the service. (W6).
Possibilities for sharing of care
The reception in the PSCC, where the users access the service to which he was sent, is a possibility of continuity of care to users of mental health services, as well as of assisted discharged. I was received very well, treated well, and recognized well; it was important for me. I felt better. I was well received, she explained a lot about the disease, told me that I would have a normal life with the medicine, working the psychological aspects, telling me that I would be able to take care of my family again. (U2); For me it was a good thing, excellent! I was in a moment that although leaving the hospital, I was not in a good moment. The way they welcomed me, surprised me! Because I never imagined I would be so well received. (U7); In some exceptional cases, we have already performed assisted discharge, which is the case when someone from here takes the patient to the PSCC on a day previously scheduled with the PSCC to ensure that the patient was at least embraced there. We made weekly visits to the PSCC taking some inpatients that we thought could be referred to the PSCC; it was a way of making the patient to get familiar with the PSCC already during hospitalization. (W6); Besides reporting that they had been embraced, the user demonstrated the importance of the service to them and the relationship established with the team. The staff was anxious, worried about me. Whenever I do crazy things, the staff gets worried: "How long have you not come here to PSCC, were you sick?" It is affection, a feeling of warmth, you know? "You have to attend the groups, you have to participate more" it is something really nice. (U1); The physical therapist talks a lot with me, she says: "it’s not just a professional who helps, there are groups that help, you have to participate". So, I come on Mondays, Tuesdays and Thursdays. (U4) I, I feel embraced. If I feel like crying, I go there and talk to the psychologist. She finds a room, anywhere, a little corner in the courtyard to talk, to hug me. (U8).
Discussion
In the search for shared care, work on mental health is permeated by intersectoriality, understood as the integrated articulation of the services that make up this network. Users can be seen as subjects that need to be recognized within society and have their demands contemplated by social networks and policies, overcoming a fragmented logic of social problems(11).
Psychosocial care is composed of a social process, complex in the constitution of its model of care. It involves user participation, review of concepts related to service practices and workers, highlighting the importance of humanized care and intersectoral dialogue in mental health(12).
Thus, in order to work on the change of a paradigm of fragmented care in the health area, it is pertinent to know the services that make up the mental health network. In order to operationalize the routing between the points of this network, attention must be paid to intersectoral dialogue(13). Currently, mental health has important challenges, such as articulation with the urgency and emergency network, communication and work with primary care, qualification and expansion of services of territorial basis, and intersectoriality in mental health actions(14).
The users themselves recognize the quality of the mental health services they access. They point out that they have flaws that compromise treatment and that can lead to psychiatric hospitalization, not to mention the current situation of difficulties related to management, referral of users, hospital re-admissions, high number of users seeking the service, and workers without qualification in the area of mental health(13,15).
These aspects corroborate with the results found in this study, regarding the challenges in the referral of users to substitute services. An example of these challenges is the lack of referral, which may be due to differences between care models. On the one hand, there is the hospital unit with a focus on drug treatment and, on the other hand, the substitute services, such as PSCC, with a view to comprehensive care and work on a territorial basis(16).
The public health care model is divided into levels of complexity of its services. Primary care acts as the main entry point into the system, being a supervisor of other services, carrying out the referral to other levels of complexity. Secondary care, in turn, consists of provision of medium-cost procedures, with services that are primarily outpatient units and substitute services, such as PSCC. Finally, tertiary care corresponds to the provision of high-cost procedures, with hospital units, including PIUs. In this perspective, a hierarchy consisting of primary, secondary and tertiary care is established(17).
Thus, in the search for shared care strategies, it is inevitable to highlight the importance of the relationships between care models in the context of mental health. However, articulating care between different levels of complexity is still challenging; it is necessary to strengthen and systematize the connection between services, so that shared care may be possible(18).
Despite differences between the care provided, communication between services must exist, whether by telephone, via letters, or digital or personal communication. However, this action should not be isolated. Users need to be guided and accompanied until the arrival in the service to which they were forwarded. This will give them opportunity of keeping and optimizing the care practices of their treatment(17).
Referral after hospital discharge is the moment when the patients receive information about post-discharge care. Thus, professionals need to know the expectations and concerns of the users, as well as the service to they are being referred. Thus, there is a hospital discharge process that needs to be based on comprehensive, intersectoral and interdisciplinary treatment, in order to offer support to users within a care network.
However, there are still health networks that are sometimes rhizomatic networks, that is, networks without defined points of entry or exit, giving way to a confusing flow(12). Within this flow, as fruits of the Brazilian Psychiatric Reform process, guided by the process of deinstitutionalization of users, there are substitute services, including the PSCCs and the Psychosocial Support Centers (PSSCs), Sheltered Homes, Coexistence Centers, Day Hospitals, and the Cooperatives, among others. These are services that go beyond treatment; they involve mental health care based on the promotion of health and well-being of users(6).
PSCC is a service based on territorial coverage, oriented by an expanded view of the context in which the users are inserted. This implies going beyond the geographical space, recognizing the individualities of each user. Thus, it is understood that comprehensive care can be strengthened by stimulating the interaction between all subjects involved in the care for people with mental disorders(18). The territorial work allows a monitoring of the reality experienced by the users. It contributes to the construction of care that overarches the difficulties of the daily life of these individuals, with the possibility of creating a practice of care adapted to the peculiarities of each patient.
In the PSCC, embracement, bonding and co-responsibility are fundamental requirements for the organization of health care. These factors build affective bonds, trust, respect and sharing of knowledge among users, family members and workers(13).
Thinking about comprehensive care to users, the importance of embracement in mental health services stands out, with the proposal of "materialization" of a meeting between users and service(16). In order to the flow of mental health patients in the network to occur effectively, it is necessary to make referrals to the substitute services during hospital discharge, and this aspect is fundamental for the bond between users and services/workers.
Re-hospitalization rates have been used as indicators of the quality of care provided in mental health. Besides bringing data of the reality in which users are inserted, they expose characteristics of the support provided by the mental health network before the singularities of users(15).
Re-hospitalizations are common during mental health treatment. Among the factors that lead to re-hospitalizations are the non-adherence to substitute services and irregular treatment. As a strategy to overcome these difficulties, there is the project of assisted discharge(19). The aim of this project is to ensure the provision of extra-hospital care by reversing the process of social exclusion of patients who leave an institution. Work is carried out with patients and family members, promoting contact with them after discharge to provide guidelines about the medication and encourage commitment to treatment adherence and to accompany the users to the referral service, seeking the commitment of the manager with the treatment of the referred users, thus helping in the construction of their link with the service.
Regarding the bonding of users with substitute mental health services, this can be directly related to the perception that the users have of the services and the treatment received in that environment. Since the embracement in the service to the beginning of their inclusion in the activities, the intersubjective relationships established between users and workers are fundamental for comprehensive care(20).
From the interaction between users and the other subjects involved in the care, the creation of bond facilitates the users’ adherence to the substitute service, which can be favored through interdisciplinary actions. These can strengthen the sharing of care among professionals, through exchanges of knowledge that aim to facilitate the construction of an adequate referral within the network(4).
Interdisciplinary actions make it possible to emancipate users in face of their real needs. This can happen through actions planned in a shared way among users and professionals from different areas. Then, a network of interdependence and co-responsibility aimed at comprehensive care and networking is created(4).
In order to achieve results in the area of mental health and consolidate the care networks based on the principles of intersectoriality, comprehensiveness and interdisciplinarity, it is important to break the traditional care model. The articulation between services and professionals must take place in a structured way, where different sectors communicate, reflect and think about the sharing of care.
Final considerations
The research made it possible to know the perceptions of users and workers about the sharing of care within the mental health network of a municipality in the state of Rio Grande do Sul. It was evidenced that there are challenges in the mental health network, such as the guidance, referral and access of users to substitute services. In addition to the challenges, the possibilities for effective sharing of care were known, precisely, the embracement, assisted discharge, and the bonding of users with substitute services.
As a strategy for the sharing of care in mental health care networks, principles such as intersectorality, comprehensiveness and interdisciplinarity stand out. Thus, care can be provided to help services to be connected in order to reduce the fragmentation of care, enabling an articulated and consolidated health network. To this end, it is necessary that the workers and managers of the services become responsible for the sharing of care, through the commitment of referral after hospital discharge and embracement in the services to which patients are referred.
The present study presents as a limitation the fact that it was performed in a microregion, thus preventing the generalization of the data. However, it is expected that the study contribute to a reflection on the psychosocial paradigm in the creation of mental health care shared between the hospital and the extra-hospital network.
Referências
1. Nasi C, Schneider JF. O centro de Atenção Psicossocial no cotidiano dos seus usuários. Rev Esc Enferm USP. 2011;45(5):1157-63. [ Links ]
2. Ministério da Saúde (BR). Política Nacional de Humanização – PNH. Brasília (DF): Ministério da Saúde; 2013.
3. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Núcleo Técnico da Política Nacional de Humanização. Humaniza SUS: Documento base para gestores e trabalhadores do SUS / Ministério da Saúde, Secretaria de Atenção à Saúde, Núcleo Técnico da Política Nacional de Humanização. 4. ed. Brasília: Editora do Ministério da Saúde; 2010. [ Links ]
4. Ferro LF, Emelin CS, Zimmermann AB, Castanharo RCT, Oliveira FRL. Interdisciplinaridade e intersetorialidade na Estratégia Saúde da Família e no Núcleo de Apoio à Saúde da Família: potencialidades e desafios. O Mundo da Saúde. 2014;38(2):129-38. [ Links ]
5. Paes LG, Schimith MD, Barboza TM, Righi LB. Rede de atenção em saúde mental na perspectiva dos coordenadores de serviços de saúde. Trab Educ Saúde. 2013;11(2):395-409. [ Links ]
6. Ramos DKR, Guimarães J, Mesquita SKC. Dificuldades da rede de saúde mental e as reinternações psiquiátricas: problematizando possíveis relações. Cogitare Enferm. [Internet]. 2014 Jul/Set [Acesso 27 nov 2016];19(3):553-60. Disponível em: http://revistas.ufpr.br/cogitare/article/view/35382. [ Links ]
7. Pessoa JM, Santos RCA, Clementino FS, Oliveira KKD, Miranda FAN. Política de saúde mental no hospital psiquiátrico: desafios e perspectivas. Esc Anna Nery. [Internet]. 2016 Jan/Mar [Acesso 21 nov 2016];20(1). Disponível em: http://www.scielo.br/pdf/ean/v20n1/1414-8145-ean-20-01-0083.pdf. [ Links ]
8. Minayo MCS. O Desafio do Conhecimento: Pesquisa Qualitativa em Saúde. 12. ed. São Paulo: Hucitec; 2014. [ Links ]
9. Fontanella BJB, Ricas J, Turato ER. Amostragem por saturação em pesquisas qualitativas em saúde: contribuições teóricas. Cad Saúde Pública. 2008;24(1):17-27. [ Links ]
10. Ministério da Saúde (BR). Conselho Nacional de Saúde. Resolução nº 466, de 12 de dezembro de 2012. Diretrizes e normas regulamentadoras de pesquisas envolvendo seres humanos. Diário Oficial da União [da] República Federativa do Brasil. 2013 jun 13;150(112 Seção 1):59-62. Brasília, 2012. [ Links ]
11. Scheffer G, Silva LG. Saúde mental, intersetorialidade e questão social: um estudo na ótica dos sujeitos. Serv Soc Soc. 2014 Apr/Jun;(118):366-93. [ Links ]
12. Vasconcelos MGF, Jorge MSB, Catrib AMF, Bezerra IC, Franco TB. Projeto terapêutico em saúde mental: práticas e processos nas dimensões constituintes da atenção psicossocial. Interface. (Botucatu). 2016;20(57):313-23. [ Links ]
13. Pessoa M Júnior, Santos RCA, Clementino FS, Oliveira KKD, Miranda FAN. A política de saúde mental no contexto do hospital psiquiátrico: desafios e perspectivas. Esc Anna Nery. 2016 Jan/Mar;20(1):83-9. doi: 10.5935/1414-8145.20160012 [ Links ]
14. Cardoso MRO, Oliveira PTR, Piani PPF. Práticas de cuidado em saúde mental na voz dos usuários de um Centro de Atenção Psicossocial do estado do Pará. Saúde Debate. 2016 Apr/Jun;40(109):86-99. [ Links ]
15. Machado V, Santos MA. O tratamento extra-hospitalar em saúde mental na perspectiva do paciente reinternado. Psicol Estud. 2013;18(4):701-12. [ Links ]
16. Ballarin MLGS, Ferigato SH, Carvalho FB, Miranda IMS. Percepção de trabalhadores de um CAPS sobre as práticas de acolhimento no serviço. O Mundo da Saúde. 2011;35(2): 162-68. [ Links ]
17. Mendes EV. As Redes de Atenção à Saúde. Brasília: Organização Pan-Americana da Saúde; 2011. [ Links ]
18. Lima MS, Aguiar ACL, Sousa MM. O cuidado compartilhado em saúde mental como potencial de autonomia do usuário. Psicol Estud. 2015;20(4):675-86. [ Links ]
19. Dimenstein M, Bezerra CG. Alta-Assistida de usuários de um hospital psiquiátrico: uma proposta em análise. Physis. 2009;19(3):829-48. [ Links ]
20. Andrade AB, Bosi MLM. Qualidade do cuidado em dois centros de atenção psicossocial sob o olhar de usuários. Saúde Soc. 2015;24(3)887-900. [ Links ]
Received: Oct 17th 2017 Corresponding
Author:
Accepted: Dec 7th 2018
Daiana Foggiato de Siqueira
E-mail: daianasiqueira@yahoo.com.br
https://orcid.org/0000-0002-8592-379X











 texto em
texto em 


